Blog
Foot Injuries in Figure Skating and What They Mean

Foot stress fractures, ankle bursitis, and lace bite are common injuries among figure skaters due to repetitive impact, tight footwear, and intense training. A foot stress fracture is a small crack in the bone that develops from repeated stress, often causing deep pain that worsens with activity. Ankle bursitis is inflammation of the fluid-filled sacs surrounding the ankle joint, leading to swelling, tenderness, and discomfort with movement. Additionally, lace bite occurs when pressure from tight skate laces irritates the tendons on the top of the foot, causing pain and inflammation. These conditions can make skating difficult and limit performance. A podiatrist can evaluate the injury, use imaging for diagnosis, and provide treatment plans to reduce pain and protect foot function. If any of the above symptoms develop from ice skating, it is suggested that you visit a podiatrist for an evaluation and appropriate care.
Ankle and foot injuries are common among athletes and in many sports. They can be caused by several problems and may be potentially serious. If you are feeling pain or think you were injured in a sporting event or when exercising, consult with one of our podiatrists from Ocotillo Foot and Ankle Centers. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Common Injuries
The most common injuries that occur in sporting activities include:
- Achilles Tendonitis
- Achilles Tendon Rupture
- Ankle Sprains
- Broken Foot
- Plantar Fasciitis
- Stress Fractures
- Turf Toe
Symptoms
Symptoms vary depending upon the injury and in some cases, there may be no symptoms at all. However, in most cases, some form of symptom is experienced. Pain, aching, burning, bruising, tenderness, tightness or stiffness, sensation loss, difficulty moving, and swelling are the most common symptoms.
Treatment
Just as symptoms vary depending upon the injury, so do treatment options. A common treatment method is known as the RICE method. This method involves rest, applying ice, compression and elevating the afflicted foot or ankle. If the injury appears to be more serious, surgery might be required, such as arthroscopic or reconstructive surgery. Lastly, rehabilitation or therapy might be needed to gain full functionality in the afflicted area. Any discomfort experienced by an athlete must be evaluated by a licensed, reputable medical professional.
If you have any questions please contact our offices located in Chandler, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Not Every Child's Heel Pain Is Sever's Disease
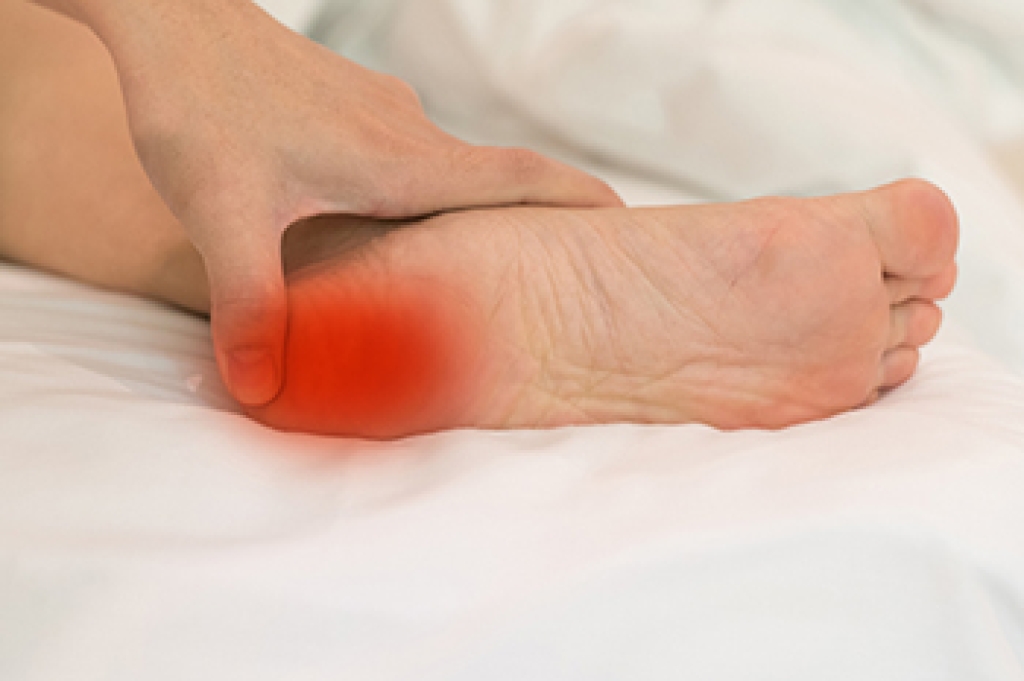
Heel pain in active children is often linked to Sever's disease, a common condition caused by irritation at the growth plate in the heel during periods of rapid growth and repeated activity. However, not every young athlete with heel pain has this condition. Similar symptoms may come from Achilles tendon strain, bone stress injuries, deep bruising, or other joint-related problems. Running, jumping, and frequent training can place repeated stress on the heel, making proper diagnosis important when pain does not improve. A podiatrist can evaluate where the pain is located, review activity history, assess walking patterns, and order imaging if needed, to identify the true cause. Running, jumping, and high impact sports can place repeated stress on the heel, making diagnosis important when pain continues. A podiatrist can evaluate the location of pain, activity history, walking pattern, and imaging if needed, to determine the exact cause. Proper diagnosis helps ensure the child receives the right treatment and avoids worsening the problem by continuing sports too soon. If your child has ongoing heel pain during athletic activity, it is suggested that you visit a podiatrist for an accurate diagnosis and effective treatment.
Many people suffer from bouts of heel pain. For more information, contact one of our podiatrists of Ocotillo Foot and Ankle Centers. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions, please feel free to contact our offices located in Chandler, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What Gout Is and Why It Affects the Big Toe
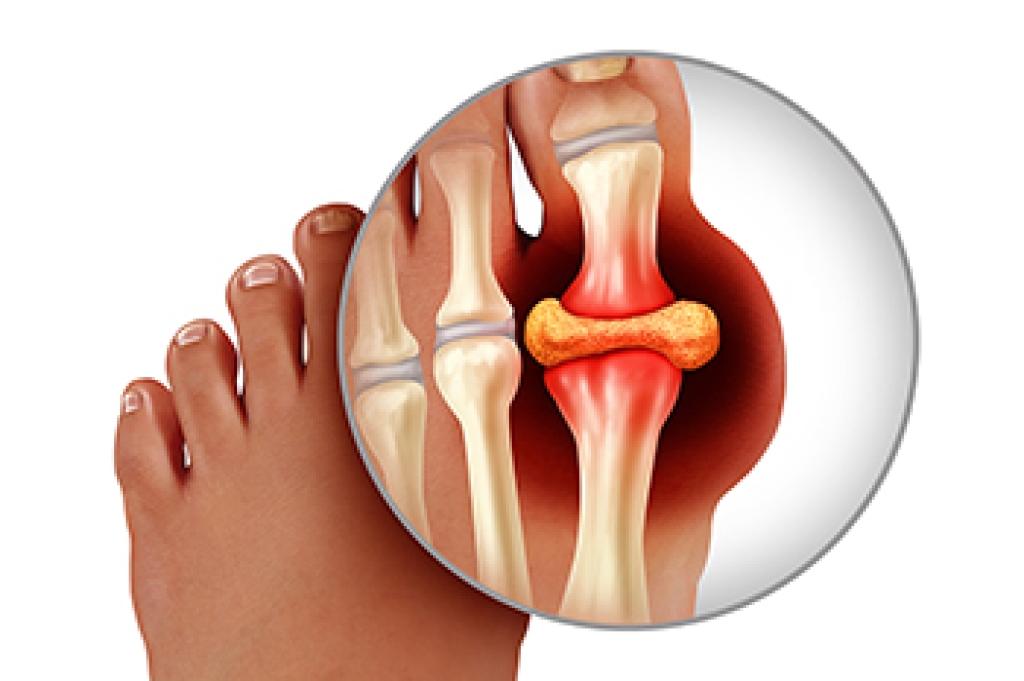
Gout is a form of inflammatory arthritis caused by a buildup of uric acid crystals in the joints. It often affects the big toe because this joint is more prone to cooler temperatures and stress, which can encourage crystal formation. Symptoms include sudden intense pain, redness, swelling, and warmth in the affected area. Flare-ups can occur suddenly and may limit movement. Risk factors include a diet high in purines, dehydration, certain medications, and underlying health conditions. A podiatrist can help manage symptoms, provide guidance on lifestyle changes, and recommend treatments to reduce inflammation and prevent future attacks. Gout can be painful and may impact daily activities. If you have had one or more gout attacks, it is suggested that you consult a podiatrist who can help you to manage this painful condition.
Gout is a painful condition that can be treated. If you are seeking treatment, contact one of our podiatrists from Ocotillo Foot and Ankle Centers. Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our offices located in Chandler, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Two Small Bones in the Foot Can Cause Big Pain
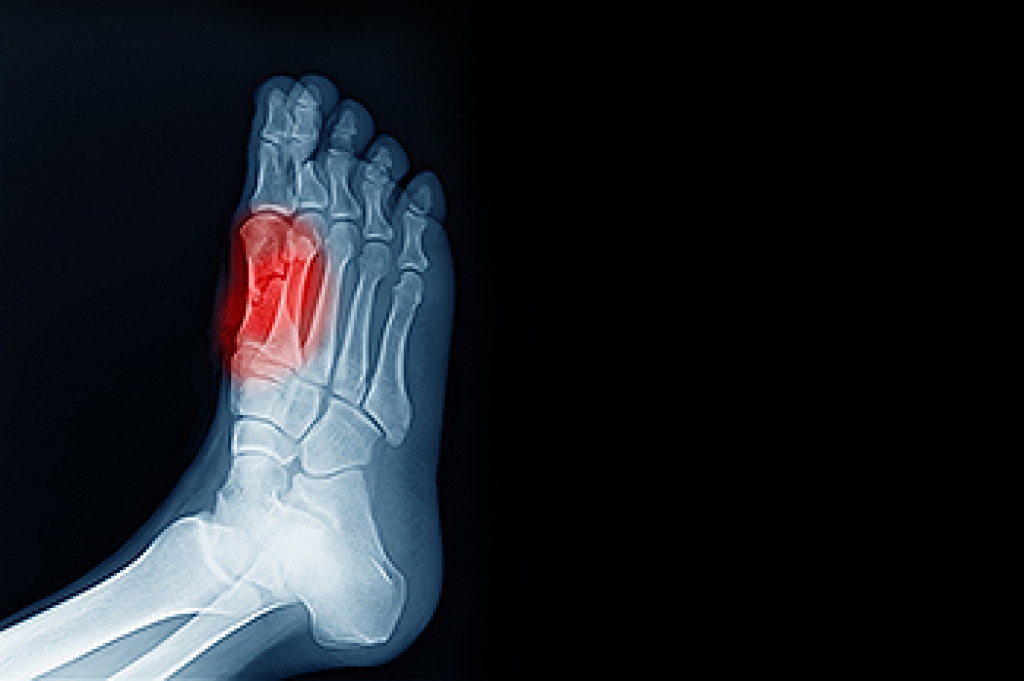
Two tiny bones under the big toe joint, called sesamoids, help the foot handle pressure while walking and running. When these bones or the surrounding tissue become irritated, inflammation can develop. This often causes pain beneath the base of the big toe, especially when walking, standing for long periods of time, or wearing thin-soled or high-heeled shoes. The area may feel swollen, warm, or tender, and bending the big toe can make the pain worse. Repeated stress from dancing, jogging, or wearing poor-fitting shoes often leads to this problem. A podiatrist can examine the foot, check for swelling, and order X-rays to rule out a fracture or arthritis. Treatment of sesamoiditis includes custom orthotics, offloading pads that reduce pressure, and supportive shoes with thicker soles. Pain also can be relieved with anti-inflammatory medicine taken orally and injections to numb the painful area. If you have pain beneath the big toe joint, it is suggested that you schedule an appointment with a podiatrist for an accurate diagnosis and effective treatment.
Sesamoiditis is an unpleasant foot condition characterized by pain in the balls of the feet. If you think you’re struggling with sesamoiditis, contact one of our podiatrists of Ocotillo Foot and Ankle Centers. Our doctors will treat your condition thoroughly and effectively.
Sesamoiditis
Sesamoiditis is a condition of the foot that affects the ball of the foot. It is more common in younger people than it is in older people. It can also occur with people who have begun a new exercise program, since their bodies are adjusting to the new physical regimen. Pain may also be caused by the inflammation of tendons surrounding the bones. It is important to seek treatment in its early stages because if you ignore the pain, this condition can lead to more serious problems such as severe irritation and bone fractures.
Causes of Sesamoiditis
- Sudden increase in activity
- Increase in physically strenuous movement without a proper warm up or build up
- Foot structure: those who have smaller, bonier feet or those with a high arch may be more susceptible
Treatment for sesamoiditis is non-invasive and simple. Doctors may recommend a strict rest period where the patient forgoes most physical activity. This will help give the patient time to heal their feet through limited activity. For serious cases, it is best to speak with your doctor to determine a treatment option that will help your specific needs.
If you have any questions, please feel free to contact our offices located in Chandler, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.